In the course of evaluating patients for GERD we often see patients who have difficulty swallowing. The “medical” term for this is dysphagia. Most of the time this is a structural issue related to a large hiatal hernia or scarring in the distal esophagus that prevents food from moving down into the stomach. However during our evaluations we do find people who have a completely different cause of their swallowing difficulty. This condition is called ACHALASIA.
Achalasia is an esophageal disorder of unknown cause characterized by a complete lack of peristalsis in the lower esophagus combined with a failure of the lower esophageal sphincter to relax appropriately. As a consequence, patients have difficulty swallowing both liquids and solids. It is a very frustrating disease for patients because the medical community can not tell the patient why it has happened to them. Abnormalities and degeneration of the nerves that are responsible for esophageal contractions and relaxation are described under the microscope but we don’t know why these nerves have become injured. Infectious etiologies or autoimmune disorders are felt to be the primary cause of the nerve injuries but proof and prevention are lacking. A form of achalasia is caused by a parasitic infection in rural Latin America. This disease is called Chagas disease and is caused by a protozoan named, Trypanosoma cruzi.
Treatment of Achalasia
Medical Management– there are no medical therapies for achalasia that has been shown to have anything more than short term efficacy. They focus on botox injections to relax the dysfunctional lower esophageal sphincter or forceful dilation of this area to rupture the muscle fibers and achieve a similar effect. Response to botox injections into the esophagus during EGD is variable but even when effective rarely lasts beyond 6 months. Dilation with specialized ballon tipped catheters can be effective in some carefully chosen patients but the perforation risk is approximately 2% so repetitive dilation is typically discouraged and unfortunately the scar from those efforts can make surgery more difficult.
Botox injections are often used in a repetitive fashion in patients that either due to age or others reasons are not felt to be safe candidates for surgery.

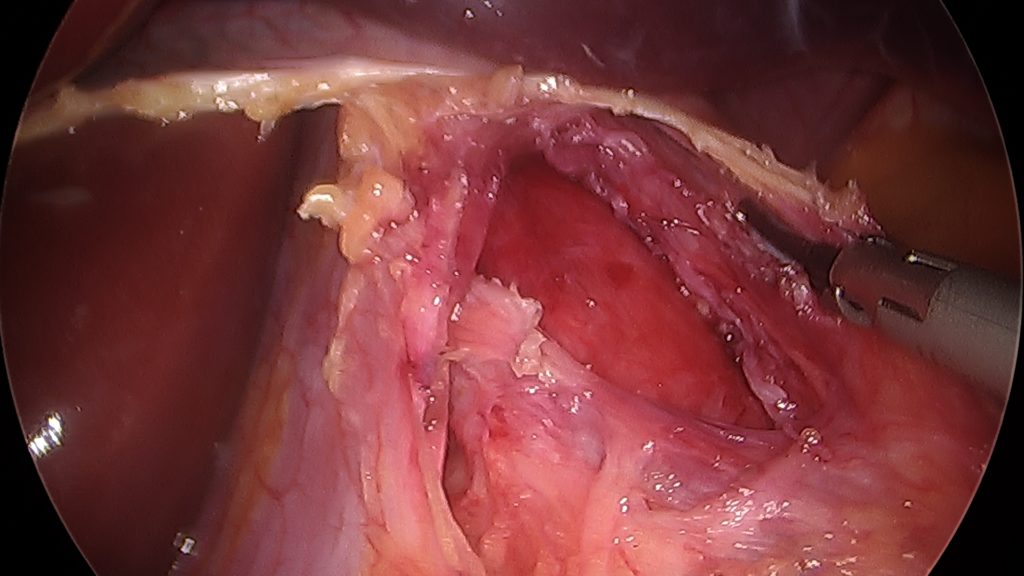

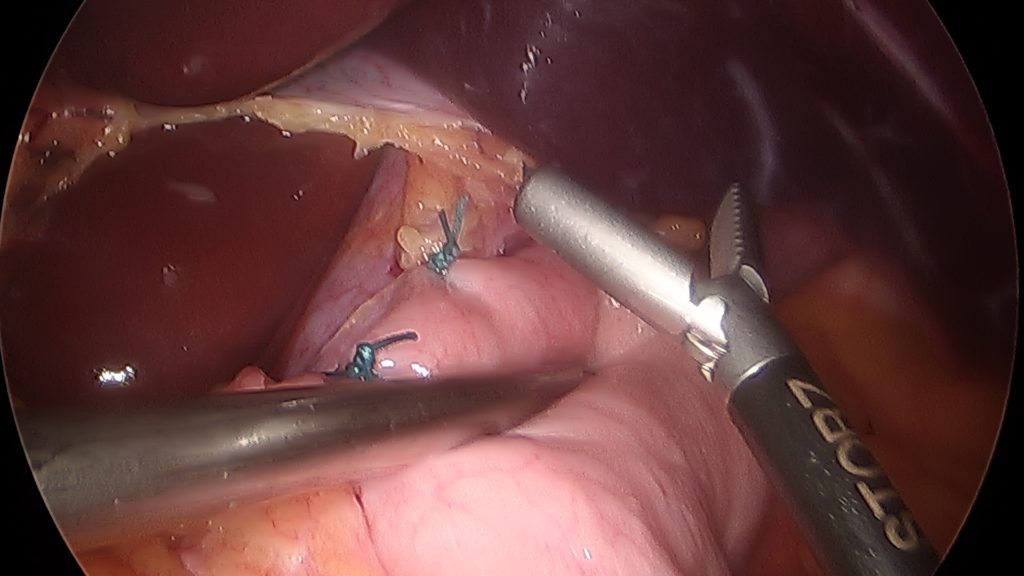
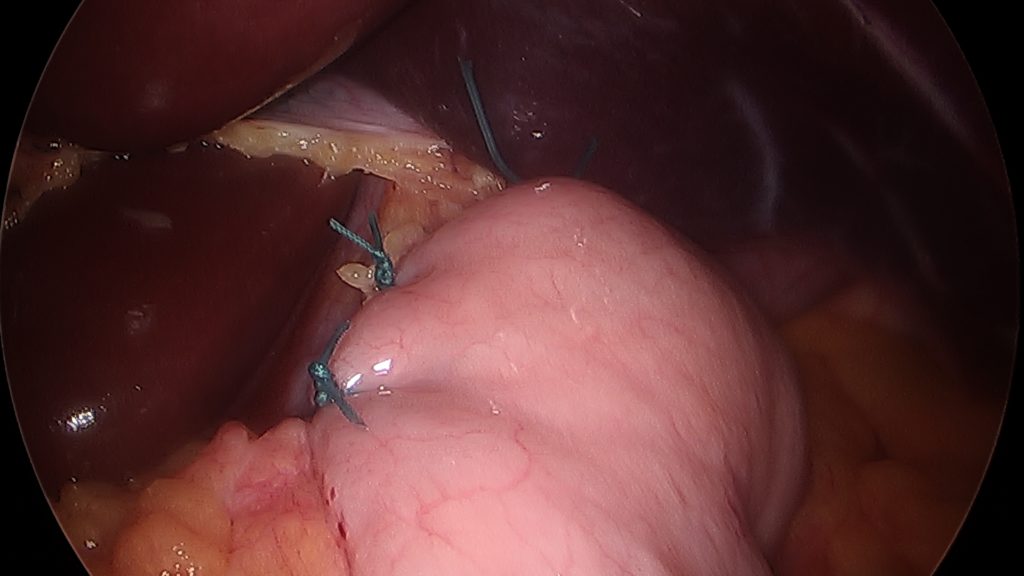
Surgical Management – The first successful surgery for Achalasia was performed by its namesake, Dr Ernest Heller in 1913. Prior to the 1990’s this surgery was performed via an thoracotomy (chest incision). Now it is typically done with laparoscopic techniques and a brief overnight stay.
The goal of the surgery into improve drainage of food and liquids from the esophagus into the stomach. We do this by cutting the dysfunctional muscles on the upper stomach and extending that cut upwards through the LES and on to the esophageal wall for a variable distance. This leaves the thin inner mucosal layer of the esophagus and stomach intact but allows the area that was previously constricted to open up significantly. Many surgeons will add a very gentle anti-refux procedure or wrap to prevent the regurgitation of fluid from the stomach back through this now incompetent valve.
This procedure, the Heller Myotomy should only be performed by surgeons with advanced laparoscopic skills as the complications related to perforations and leaks in the esophagus are significant. The long term success rate of this procedure in appropriate hands is approximately 90%.
Most Common Symptoms of Achalasia
Dysphagia (trouble swallowing)
Regurgiation
Weight loss
Chest pain
Heartburn
Cough
Diagnosis of Achalasia
Patients history is often classic with progressive difficulty with swallowing liquids and solids over a long period.
Xray and Barium Swallow may show a dilated esophagus and a “birds beak” deformity at the junction of the stomach and esophagus (LES) but these changes occur long after the swallowing problems start.
Endoscopy may reveal residual food and fluid in the esophagus with a tight junction between the stomach and esophagus that is hard to push through. Again these are late findings.
Esophageal Function Testing or “manometry” is the gold standard for diagnosis and confirms a lack of peristalsis in the esophagus.
